In recent years, there has been an increase in cases of Legionnaires’ disease worldwide, with reported incidences of Legionnaires’ disease growing at an alarming rate. In the USA alone, cases of Legionnaires’ disease have increased by over 450% since 2000 9. Similarly, between 2000 and 2015 cases of infection in Europe have risen by 347% and 2017 saw the largest ever number of reported cases (9238) and deaths (574). 14
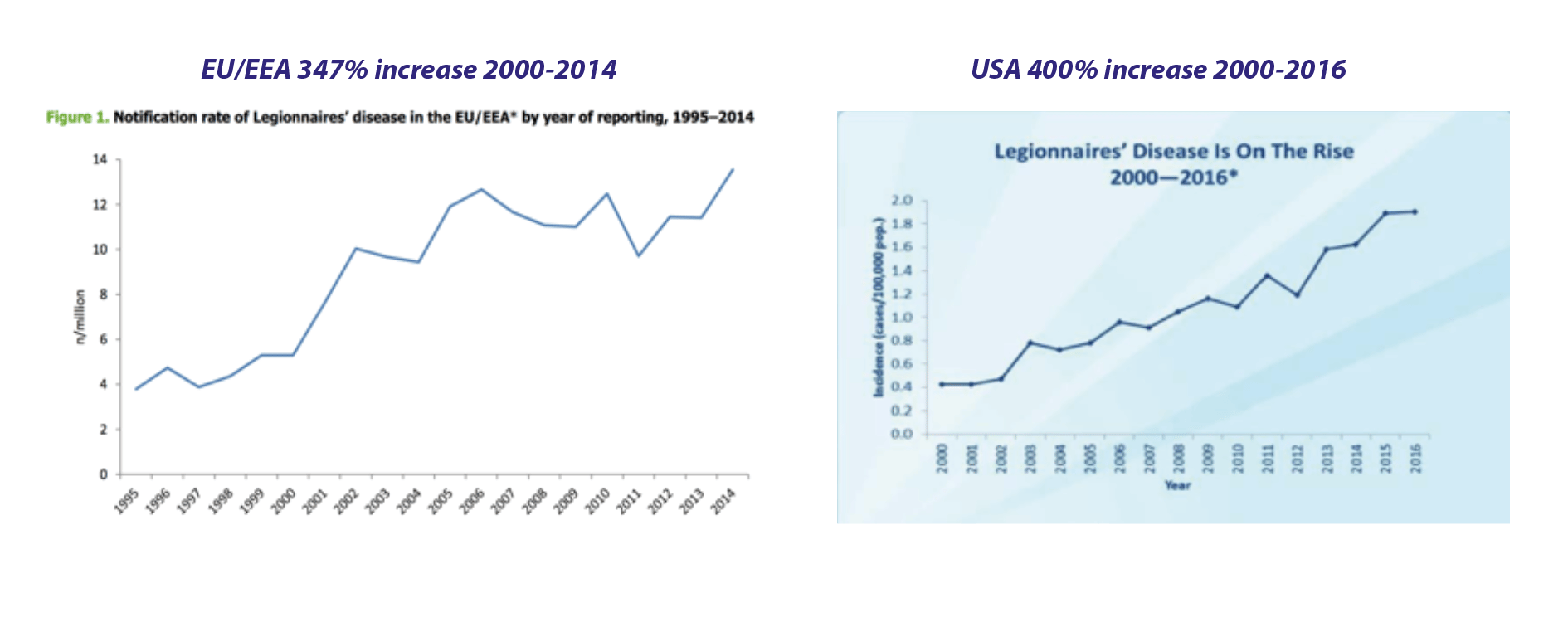
But why are incidences of this deadly disease increasing so rapidly?
Climate change
Legionnaires’ disease is caused by inhalation of aerosols (fine particles or droplets), containing Legionella bacteria. Legionella bacteria naturally occur in ponds, rivers and other natural water systems. But when the bacterium enters water systems in the built environment, conditions - such as water temperature of 25–42 °C - can often favour and encourage rapid growth and lead to explosive outbreaks of Legionnaires’ disease and other related infections.
Find Out More About Legionella and Legionnaires' disease.
This pattern of growth and transmission means that the disease is likely to be affected by weather and climate. Global warming, resulting in higher temperatures around the globe, has contributed to the increased incidences of Legionnaires’ disease worldwide. So much so that a recent paper, published in a World Health Organisation (WHO) Bulletin, argued that “Legionnaires’ disease should now be added to the Intergovernmental Panel on Climate Change (IPCC) list of important climate sensitive health issues”. 1
-
Increased Rainfalls
Several studies have identified statistically significant increases in the risk of legionellosis with increased rainfall.3 4 5 6 A study published in The Journal of Infectious Diseases found that legionellosis was associated with rainfall 6–10 days before disease onset. 2 This timing corresponds to the period between exposure to the pathogen and the development of symptoms. Another study on Legionella in rainwater on roads in Japan indicates that Legionella pneumophilais often present in puddles of rainwater on asphalt roads, especially during warm weather. 15

The researches argue thatrainfall might affect exposure to Legionella, via a range of potential mechanisms. Contamination of reticulated drinking water is one possibility.7Another suggestion is that vehicles might produce aerosols containing Legionella, as they drive on wet road surfaces. 5 8 The general public can the get infected by inhaling these aerosols. The study suggests that molecular matching of clinical and environmental samples provides strong support for this hypothesis. 5 8
-
Rising Sea Water Levels
Besides the effect of the rainfall and high temperatures on the growth of Legionella, there are other potential growth sources for this bacterium due to climate change. Higher temperatures impact sea water levels and increase flood risks. Since Legionella can be found in natural bodies of water, this could increase the Legionella bacterial count in soil. 10

-
Increased use of cooling systems
Warmer temperatures are accompanied by a spike in the use of air-conditioning units and cooling systems. However, when they are not properly maintained, they provide the perfect environment for Legionella to become mobile and airborne.

The study of Outbreaks of Legionnaires disease Caused by Long‐Distance Spread suggests that in some cases Legionella can travel as far as 10 km 11. If aerosols created by air-conditioning units or cooling towers are contaminated with Legionella they can pose a real threat to people in the area. In fact, Legionella was first discovered when 29 out of the 182-people infected died due to poor maintenance of a hotel cooling tower in Philadelphia.
Aging Population
Our rapidly changing population is driven prodemenantly by two factors. The first being prolonged life expectancy, driven by improvements in healthcare and lifestyles ,and the second being a global decrease in fertility as people opt to have fewer children or to have children later in life12.
In 2010, an estimated 524 million people were aged 65 or over – 8 % of the world’s population. By 2050, this number is expected to nearly triple to about 1.5 billion14.According to the WHO we will soon have more elderly people than children and more people at an extreme old age than ever before 13.

A rapidly growing aging population means that an increased number of people will have weaker immune systems and illnesses such as respiratory problems, kidney disease, diabetes or cancer. Although anyone can catch Legionnaires’ disease, the elderly and those with weakened immune systems, are more prone to catching the infection and are less likely to resond to medical attention. As a result, cases of Legionnaires’ disease and deaths from the infection are expected to increace globally.
Better diagnostics
Legionnaires disease is often perceived to be a rare form of infection however, its is more common than most people realise. According to CDC,Health departments in the US reported almost 7,500 cases of Legionnaires’ disease in 2017. 9 Similarly, in Europe 9,238 cases were reported in 2017- this is the highest number ever observed, a notable increase when compared with 2016.14
One major reaon for this perceived rarity is missdiagnosis. Unless special tests are performed - such as a traditional lab based techniques or rapid urine antigen testing – the non-specific symptoms of Legionnaires’ disease can be confused for something else. And because Legionnaires’ disease is perceptively rare, doctors seldom push for specific testing for their patients.
Nonetheless, in more recent years, hospitals and healthcare facilities, in the developed countries especially, have started to recognize the importance of diagnostic testing for Legionella in order to improve the accuracy of their diagnosis. As a result, more cases are now being reported every year, which has contributed to the overall increase in incidences of Legionnaires’ disease worldwide.
How to minimise risk of Legionella?
Because Legionella is so pervasive, and complete eradication of the bug is almost impossible, it is vital that strong control measures are supplemented with regular testing. However, concerns have been raised about the reliability of traditional testing methods in protecting public health. For instance, Research in 2014 by Whiley and Taylor saw almost 4,000 environmental samples analysed for Legionella, with 34% of samples testing positive when ‘culture methods’ were used but 72% testing positive when using a quantitative polymerase chain reaction (qPCR) method16.
Considering the rapid increase of cases of Legionnaires’ disease worldwide, it is crucial that water management professionals and duty holders use new innovative testing techniques to protect against the limitations of widely accepted testing methods, like lab culture, and to minimise the risk of Legionella in their facilities.
New rapid testing methods, such as the Hydrosense antigen test, allow anyone to detect dangerous Viable-but-non-Culturable Legionella when the culture method is unable to and to recive results on-site almost immediately (25 minutes, compared to 10-14 days with traditional methods). The ability to
know instantly if a water system is infected with Legionella, gives duty holders the power to act quickly and ensure that the water system is treated before anyone gets infected.
Find out more about key testing methods for Legionella available on the market.
References
- Sakamoto, R. (2015). Available at: http://bit.ly/2m1OAQR [Accessed: 08 Feb. 2019].
- Fisman D.N., Lim S., Wellenius G.A., Johnson C., Britz P., Gaskins M., (2005). Journal of Infectious Diseases. Available at: http://bit.ly/2mgN0L9 [Accessed 08 Feb. 2019].
- Hicks L.A., Rose C.E., Fields B.S., Drees M.L., Engel J.P., Jenkins P.R. (2007). Available at: http://bit.ly/2m1OLeZ [Accessed 08 Feb. 2019].
- Garcia-Vidal C., Labori M., Viasus D., Simonetti A., Garcia-Somoza D., Dorca J. (2013). Available at: http://bit.ly/2m1OSXX [Accessed 08 Feb. 2019].
- Chen N.T., Chen M.J., Guo C.Y., Chen K.T., Su H.J (2014). Available at : http://bit.ly/2kng3Mv [Accessed: 08 Feb. 2019].
- Halsby K.D., Joseph C.A., Lee J.V., Wilkinson P. (2014). Available at: http://bit.ly/2miiFMd [Accessed 06 Feb. 2019].
- Falkinham J.O. 3rd, Hilborn E.D., Arduino M.J., Pruden A., Edwards M.A. (2015). Environmental Health Prospectus. Available at: http://bit.ly/2kPVVCU [Accessed : 08 Feb. 2019].
- Sakamoto R., Ohno A., Nakahara T., Satomura K., Iwanaga S., Kouyama Y. (2009). Available at: http://bit.ly/2kGpVRX [Accessed 08 Feb. 2019].
- Cdc USA (2018). Available at: http://bit.ly/2kQ2OEg [Accessed 30 May. 2018].
- Water News Europe. (2017). Available at: http://bit.ly/2knVOON [Accessed 07. 2019].
- Nygård K., Werner-Johansen Ø., Rønsen S., Caugant D.A., Simonsen Ø., Kanestrøm, Eirik Ask A., Ringstad J., Ødegård R., Jensen T., Krogh T., Høiby E. A., Ragnhildstveit E., Aaberge I.S., Aavitsland P. (2008). Clinical Infectious Diseases, Volume 46, Issue 1, 1 Pages 61–69. Available at: http://bit.ly/2kQFxSM [Accessed 03 Oct. 2018].
- Office for National Statistics (2018). Available at: http://bit.ly/2knhw5t [Accessed 08 Feb. 2019].
- WHO. (2011). Available at: http://bit.ly/2kGxQPb [Accessed: 08 Feb. 2019].
- ECDC. (2018). SURVEILLANCE REPORT. Available at: http://bit.ly/2lXQ8eP [Accessed: 08 Feb. 2019].
- Sakamoto R., Ohno A., Nakahara A., Satomura K., Iwanaga S., Kouyama Y., Kura F., Kato, Matsubayashi N. Z., Okumiya K., and Yamaguchi K. (2009). Emerging Infectious Diseases. Available at: http://bit.ly/2ko2xIF [Accessed 08 Feb. 2019].
- Cox S. (2017).Brunel University of London. Available at: http://bit.ly/2mikqch [Accessed : 11 Feb. 2019].

